In the News
Elvin Ng’s eye surgery: Retinal detachment, myopia and the warning signs you should not ignore
What is retinal detachment and how is it linked to severe myopia? Experts break down why it happens, the telltale symptoms and why urgent treatment is critical.
20 March 2026
Share
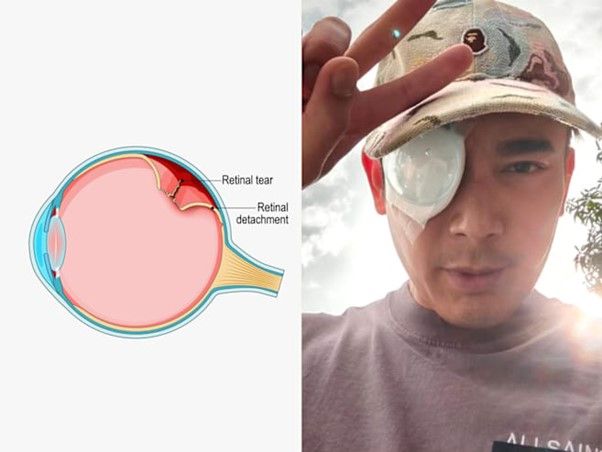
Image source: CNA lifestyle website
Blurry far vision, glasses and contact lenses – short-sighted Singaporeans are more than familiar with this myopia starter pack. But what can also potentially turn up like an unpopular Labubu in a blind box reveal is an eye condition that many myopes may not be aware of: retinal detachment.
That was what Mediacorp actor and myope Elvin Ng was diagnosed with on Feb 23 2026 after consulting a doctor about “a dark circular shadow at the bottom corner of my right eye”, he wrote on an Instagram post.
The 45-year-old actor noted that “when I moved my eye around, the shadow didn't move” and “by the evening, the shadow had covered nearly half my eye and was near the centre”.
When interviewed by 8 Days and asked if he knew what the cause of the detachment was, the actor said, “it is most likely due to my myopia as retinal detachment can happen with those with high myopia”.
Ng was scheduled for an emergency eye operation on the very same day, and a gas bubble was inserted into his affected right eye to save his vision.
Image source: Elvin Ng’s Instagram account
If you thought the treatment was unusual, wait till you read about his home-rest instructions – he had to lie face down for two weeks and could only take hourly breaks to clean his eye and take medication. “Even when I sleep, I can’t be on my back and need to face down,” he told 8 Days.
Just what is retinal detachment and can it happen to you if you have myopia? Would you also experience seeing “shadows” like Ng did if it happens to you?
CNA Lifestyle interviewed Dr Paul Zhao, the senior consultant ophthalmologist at Eagle Eye Centre, who treated Ng's retinal detachment, to find out more about the specific eye condition.
1. In Singapore, what are the common causes of retinal detachment for adults around Elvin’s age? In your practice, how often do you come across similar cases?
The most common cause of a retina detachment in adults is due to a retina tear. Patients with high myopia tend to have a higher risk as they often have areas of thinner retina which are more susceptible to tears.
Frequent eye rubbing and any trauma to the eye can also cause retina tears which if not treated promptly will progress to a retina detachment requiring major surgery.
If a retina tear is detected early during an eye exam, a relatively quick and non-invasive laser treatment can be done to prevent it from progressing to a retina detachment.
In my clinical practice, which predominantly focuses on retina conditions, I see an average of about 2-3 patients a week with retina tears or retina detachments cases.
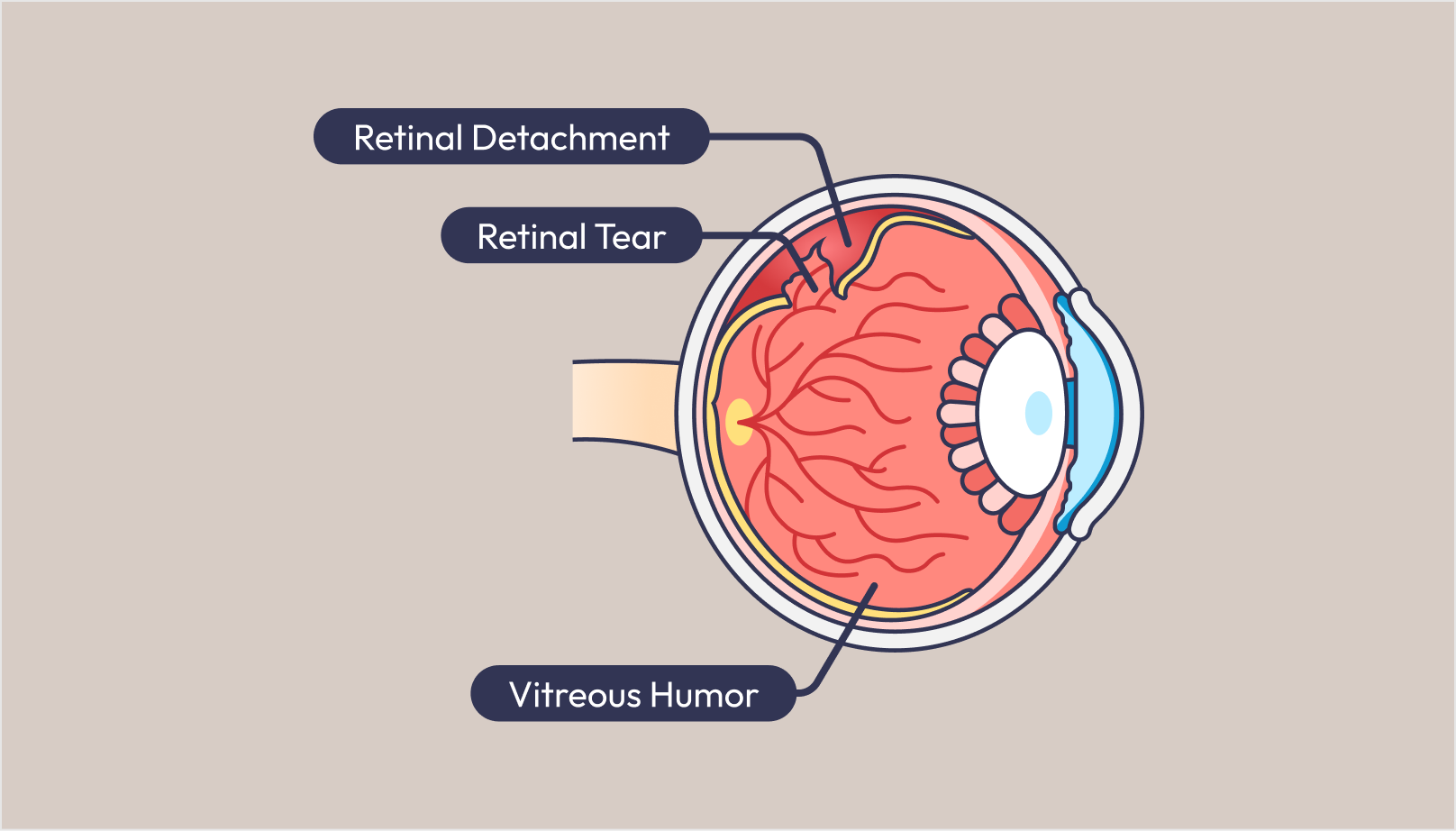
2. What is considered severe myopia? How does severe myopia contribute to retinal detachment?
The most common cause of a retina detachment in adults is due to a retina tear. Patients with high myopia tend to have a higher risk as they often have areas of thinner retina which are more susceptible to tears.
Frequent eye rubbing and any trauma to the eye can also cause retina tears which if not treated promptly will progress to a retina detachment requiring major surgery.
If a retina tear is detected early during an eye exam, a relatively quick and non-invasive laser treatment can be done to prevent it from progressing to a retina detachment.
In my clinical practice, which predominantly focuses on retina conditions, I see an average of about 2-3 patients a week with retina tears or retina detachments cases.
3. Many Singaporeans are myopic, which could potentially lead to retinal detachment. Why do we not have more people with retinal detachment?
Retina tears and retina detachment are certainly more common in Singapore than compared to a Caucasian population due to the high prevalence of myopia. The incidence of retina detachment is between 10-20 cases per 100,000 people and remains as a leading cause of sudden loss of vision. Recognising the warning signs of a retina tear and getting an eye check is crucial to preventing a retina detachment.
4. Why are floaters a sign of retinal detachment? What changes in the eye result in us seeing floaters? Other than floaters and seeing dark patches, what other signs we should not ignore?
When there is a tear in the retina, the fine blood vessels of the retina bleed and release hundreds of tiny red blood cells and pigment into the cavity of the eye. This is seen as a sudden onset of floaters or like a cloud of dust or shadow moving across your vision. Other warning signs not to ignore would be seeing flashes of light sudden blurred or distorted vision. Experiencing any of these symptoms should prompt an urgent eye assessment because early treatment can prevent permanent vision loss.
5. How much time do patients usually have from the onset of symptoms to surgery to save their vision?
This depends. If the central retina (the macula) that serves our central vision is not yet affected, we need to do the surgery before the detachment reaches the macula. For detachements in the upper half of the retina, this tends to progress more quickly as gravity pushes the fluid under the retina down towards the centre more quickly.
6. How is the surgery done ie. under local or general anaesthesia
For straightforward cases requiring only a vitrectomy, I usually do it under local anaesthesia with sedation. However, for younger patients who tend to become restless under sedation and the risk of general anaesthesia (GA) is low, I would often prefer GA. If a scleral buckle (an external silicone band around the eye) is required or I expect the surgery to be longer, I would do it under general anaesthesia.
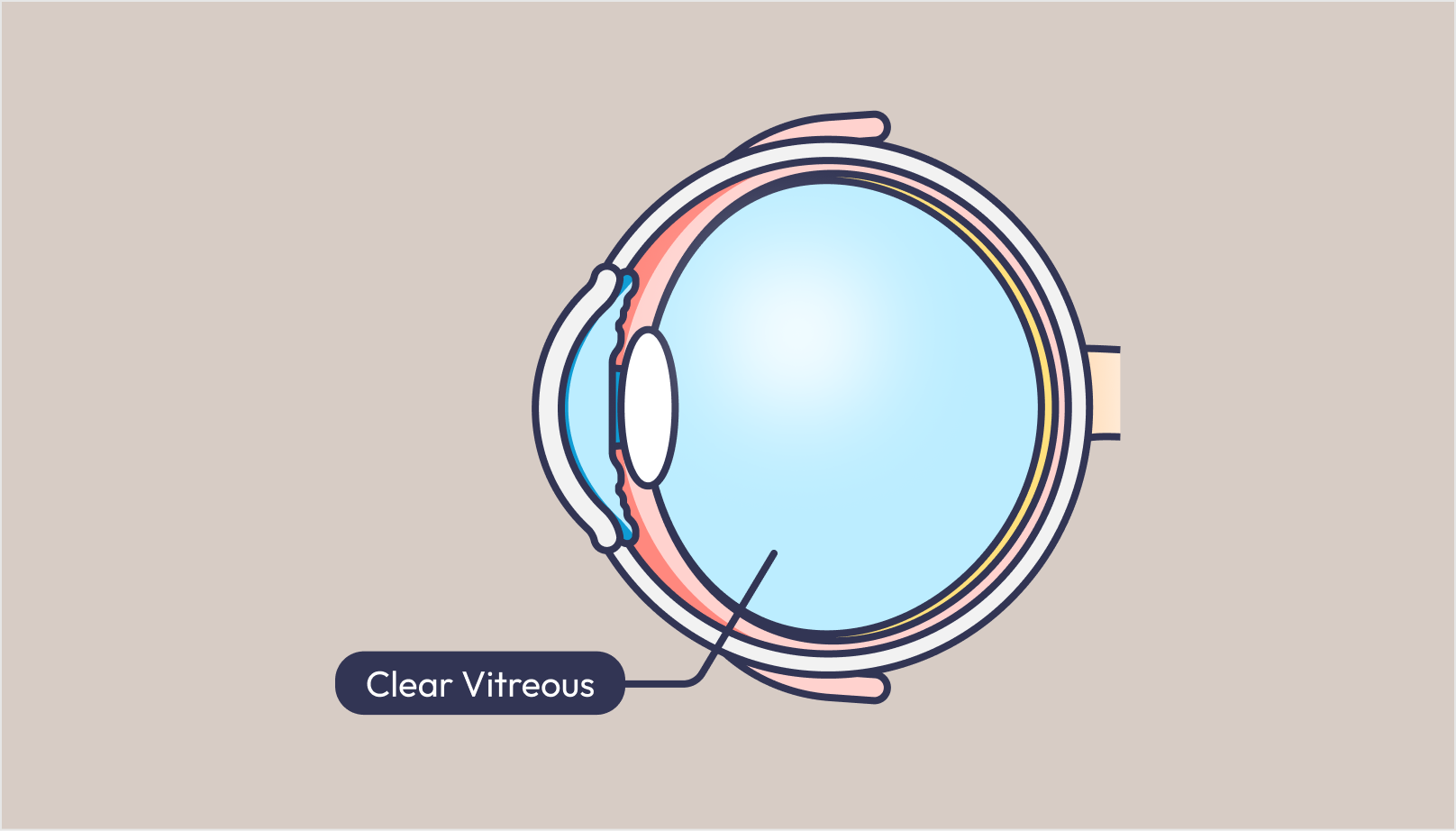
7. What is the function of the gas bubble inserted into the eye? How does the bubble reattach the retina? How is it inserted?
A vitrectomy procedure is commonly performed for retinal detachment. At the end of the procedure, the eye is filled with a gas bubble which acts like an internal bandage after removing the vitreous gel from the eye cavity to flatten the retina against the wall of the eye and preventing fluid from entering through the retina break. Laser is then applied around the edges of the hole to seal and reinforce the edges of the hole which allows the retina to recover.
8. Which part of the eye is the bubble located in the eye? Will it remain there for good or will it dissolve over time?
The gas bubble will be absorbed by the eye. Depending on the type of gas inserted, this can range from 2 weeks to 8 weeks.
9. Why does the patient have to recover lying face down? Elvin mentioned he has to lie that way for 2 weeks, with a break allowed every hour or so. Is this typical for most patients? Are there medications patients have to take and if so, what are they?
Patient’s with a gas bubble in the eye have to posture face down so that the gas bubble can float up and press on the retina which is at the back of the eye. It also prevents the gas bubble from touching the lens in front which can lead to a cataract. (clouding of the lens)
10. Can retinal detachment recur?
Yes. It can recur. Either due to new breaks forming or due to scarring which is more common in younger patients.
11. What are your thoughts on using ChatGPT to diagnose oneself?
Patients increasingly are using ChatGPT to self-diagnose and find out more about their symptoms. I have noticed patients coming earlier to see me for symptoms of floaters after googling or checking their symptoms on ChatGPT. If this enables patients to present earlier and receive more timely treatment then it would only be beneficial. At the same time, I would also caution against trusting everything that a patient reads from ChatGPT. I strongly encourage anyone experiencing symptoms to consult an eye specialist and undergo a comprehensive retinal examination. An accurate diagnosis is essential to ensure timely treatment and proper guidance on managing their eye health
Don't overlook changes in your vision. Subtle or sudden visual changes can sometimes signal a retinal problem that requires medical attention. While not every symptom is serious, timely evaluation provides clarity and allows appropriate treatment if needed. If your vision feels different from normal, it is worth having it assessed by an eye specialist.
To find out more, visit https://www.eagleeyecentre.com.sg/conditions/retinal-detachment
This article was originally published on CNA Lifestyle, and was subsequently adapted and medically reviewed by Dr Paul Zhao, Senior Consultant Ophthalmologist at Eagle Eye Centre, for HMI Medical’s website.



